
Why Choose Us

366
Licensed
Beds
Beds
21
Medical
Specialties
Specialties
213
Specialist
Doctors
Doctors
7
Centres of
Excellence
Excellence
333,870
Patient Served
Per Year
Per Year
200
Parking
Bays
Bays
Our Specialties
Gleneagles strives to bring you the best in medical care, covering a wide and diverse range of medical specialties and procedures. Discover the medical and clinical services we have available.
View All Specialties

Cardiology
A medical category specialising with disorders of the heart, cadiology is a field that includes diagnosis and treatment of congenital heart defects and other heart-related diseases. Cardiologologists are physicians who specialise in this particular field of medicine.
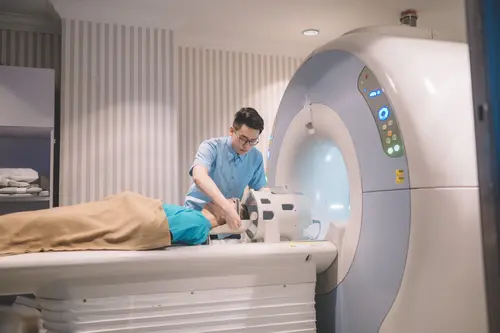
Oncology
Gleneagles Hospital medical oncology specialist centre has what it takes to provide a holistic approach in assisting and advising patients on the various aspects related to cancer care from treatment options to its side effects as well as pre- and post-treatment lifestyle changes and care.

Orthopaedic & Trauma Surgery
These are two areas of specialisation are often related as they can be caused by trauma, accidents, sports injuries, degenerative diseases, infections, tumors and congenital disorders. Orthopaedic specialists deal with conditions involving the musculoskeletal system and may use both invasive surgical and non-invasive as well as non-surgical means to correct and treat the problem.

General Surgery
This surgical specialty that focuses on abdominal organs from the intestines to the esophagus, stomach, small bowel, colon, liver, pancreas, gallbladder, bile ducts and thyroid. Though surgeons may sub-specialise in one or more of these areas using various methods such as laparoscopic surgery, they are still considered to be part of the general surgical team. These specialist surgeons are experts in treating ailments and diseases in the major body systems including cardiovascular, digestive, endocrine, excretory, skin, muscular, nervous, reproductive, respiratory and skeletal functions.

Paediatrics
Paediatricians are concerned with the care of infants, children and early adolescents. Paediatricians are often the primary care physicians from the birth of a child to caring for their health as well as general growth and well-being, including administering inoculations and vaccinations as and when necessary.

Obstetrics and Gynaecology (O&G)
Obstetrics and gynaecology are two surgical medical specialties dealing with female reproductive health and organs in pregnant (obstetrics) and non-pregnant (gynaecology) women. O&G specialists cover both areas of specialties including childbirth and delivery, as well as women's general health of the female reproductive system.
Doctors
A professional team of highly experienced doctors and specialists are available to deliver consultations and treatment plans tailored to your needs.
Our Facilities & Services
Latest Packages & Promotions

Umrah & Hajj Package 2024
Embark on your spiritual journey with ease!
Gleneagles Hospital Kuala Lumpur
01/04/2024 - 31/12/2024

Immigration Check-up
Gleneagles Hospital Kuala Lumpur offers immigration medical check-up which is required by certain country for VISA clearance.
Gleneagles Hospital Kuala Lumpur
18/06/2021 - 31/12/2024
Ward
General Ward: 9.00am to 9.00pm Intensive Care Unit (ICU) / Coronary Care Unit (CCU) / High Dependency Units (HDU) / Paediatric Ward: 12.00pm - 2.00pm (1st Session) & 5.00pm - 8.00pm (Second Session) |
COVID-19 Related Ward and Intensive Care Unit
| Monday – Sunday: No Visitor |
O'Briens Irish Sandwich Cafe
- Block B, Ground Floor
Retail Pharmacy
- MOB Specialist Clinics, Ground Floor
CIMB Bank
- Block B, Ground Floor
Retail Pharmacy
- Block B, 1st Floor
Vending Machines
- Block A, Ground Floor
Wariyaasi Kitchen
- Block B, 1st Floor
Eye Essentials
- Block A, Ground Floor
CIMB & Maybank ATM
- Block A, Ground Floor
Dome Cafe
- Block A, Ground Floor
FlowerHub
- Block A, Ground Floor
Health Market
- MOB Specialist Clinics, Ground Floor
FamilyMart
- Block B, Ground Floor
Sisters Crispy Popiah
- Block B, 1st Floor
Newslink Enterprise
- Block A, Ground Floor
Borders
- Block B, Ground Floor
Charms Cafe
- Block B, Ground Floor
Glen Cafe
- Block A, Ground Floor
Starbucks Coffee
- Block A, Ground Floor
Vagromart
- Block B, 1st Floor
Sidewalk Cafe
- Block A, Ground Floor
Madtruck Xpress
- Block B, 1st Floor
Gleneagles Hospital Kuala Lumpur

Gleneagles Hospital Kuala Lumpur (GKL) is one of the leading private hospitals in Malaysia's metropolitan capital of Kuala Lumpur and is a 376-bedded hospital that offers patients a comfortable ambience with outstanding medical care. A part of IHH Healthcare, GKL has grown into a highly respected and reputable healthcare service provider in Malaysia and the Southeast Asian region; providing excellent professional healthcare services to local and international patients.
Since 1996, GKL has provided high-quality healthcare, complemented by friendly and professional staff. As we strive to deliver excellent healthcare and patient services to our community, a good measure of our performance is recognised in the form of awards and accreditation by third-party institutions. GKL was one of the first private hospitals in Malaysia to be accredited by the US-based Joint Commission International (JCI); while locally we are accredited by the Malaysian Society for Quality in Health (MSQH). In addition, other recent notable awards that attest to the quality of care at GKL include:
- Hospital of the Year in Malaysia by GlobalHealth Asia-Pacific 2022
- Value-Based Hospital of the Year in the Asia-Pacific by GlobalHealth Asia-Pacific 2022
- Bariatric Service Provider of the Year in the Asia-Pacific by GlobalHealth Asia-Pacific 2022
- Endocrinology Service Provider of the Year by GlobalHealth Asia-Pacific 2022
GKL meets those standards by constantly upgrading our hospital facilities, often investing in cutting-edge technology that sets us apart from the rest. GKL is committed to the provision of safe and quality healthcare and is proud to have a team of highly qualified and experienced medical professionals, consultants, and nurses who go the extra mile to ensure an exceptional patient experience.
GKL is also home to some of the most advanced medical technologies and procedures available such as:
Gamma Knife Radiosurgery – A breakthrough in the medical field; as way to treat not only brain tumours but also vascular malformations and functional disorders through a minimally invasive way. The treatment procedure is simple, painless, straightforward and provides better outcomes as compared to traditional brain surgery.
Da Vinci Si Surgical System – A surgical platform designed to enable complex surgery by using a minimally invasive approach. Powered by robotic technology, Da Vinci Si surgical system allows surgeons to perform intricate surgeries with utmost meticulousness.
Download our E-Corporate Brochure here: https://online.flippingbook.com/view/176133662/
MESSAGE FROM CEO
Hoo Ling Lee
Chief Executive Officer
As the Chief Executive Officer, it is an honour to welcome you on behalf of our dedicated physicians and healthcare professionals who work together to promote essential healthcare services at Gleneagles Hospital Kuala Lumpur.
Gleneagles Hospital Kuala Lumpur has come a long way since its humble beginnings in 1996 and our growth has been made possible through the love and support that you, the community and our staff have provided over the years. I would like to express my sincere gratitude for helping us along this journey. The support we have received has made an incredible difference to Gleneagles as an organisation and to the thousands of people who we attend to every single day.
As a hospital, we feel a strong sense of duty and commitment to the people who put their faith in us. Throughout the years, Gleneagles Hospital Kuala Lumpur has proven to be resourceful, capable, and more focused than ever in keeping with our mission of making a difference in people’s lives through excellent patient care.
Each new day brings exciting advancements and technological innovations in healthcare. Gleneagles Hospital Kuala Lumpur pledges to continue building on our capabilities to ensure that we cater to the needs of our community. We will improve our facilities in line with the latest medical technology to remain committed to delivering high-quality patient care. At the same time, we will work towards implementing more sustainable measures as part of our efforts to give back to the community by applying best practices within our organisation and being a positive example in the healthcare industry.
As we move towards the future together, I consider it a great privilege to work with such an exceptional team of people who are passionate about providing the best care to our patients and their families.
We at Gleneagles Hospital Kuala Lumpur will be with you every step of the way in your time of need.
Hoo Ling Lee
Chief Executive Officer
Gleneagles Hospital Kuala Lumpur
Accreditation
2019: Joint Commission International (JCI)
2019: Malaysian Society for Quality in Health (MSQH) accreditation
2016: Joint Commission International (JCI)
2015: Malaysian Society for Quality in Health (MSQH) accreditation
2013: Joint Commission International (JCI)
2012: Malaysian Society for Quality in Health (MSQH) accreditation
2010: Joint Commission International (JCI) accreditation
2009: Organisational member of International Standard on Quality (ISQua)
2009: Malaysian Society for Quality in Health (MSQH) accreditation
2006: Malaysian Society for Quality in Health (MSQH) accreditation
2003: Malaysian Society for Quality in Health (MSQH) accreditation
2001: International Organisation for Standardisation (ISO) 9001:2000 certification
Awards
2022: GlobalHealth Asia-Pacific Awards 2022 (Hospital of the Year in Malaysia)
2022: GlobalHealth Asia-Pacific Awards 2022 (Value Based Hospital of the Year)
2022: GlobalHealth Asia-Pacific Awards 2022 (Bariatric Service Provider of the Year)
2022: GlobalHealth Asia-Pacific Awards 2022 (Endocrinology Service Provider of the Year)
2022: The Edge Malaysia Best Managed & Sustainable Property Awards (Special Mention)
2021: GlobalHealth Asia-Pacific Awards 2021 (Value Based Hospital of the Year)
2021: GlobalHealth Asia-Pacific Awards 2021 (Diabetes Service Provider of the Year)
2021: GlobalHealth Asia-Pacific Awards 2021 (Endocrinology Service Provider of the Year)
2020: GlobalHealth Asia-Pacific Awards 2020 (Bariatric Service Provider of the Year)
2019: GlobalHealth & Travel Awards (Urology Service Provider of the Year)
2019: GlobalHealth & Travel Awards (Health Screening Provider of the Year)
2018: IMTJ Medical Travel Awards for International Hospital of The Year – Winner
2018: IMTJ Medical Travel Awards for Excellence in Customer Service – Highly Commended
2018: IMTJ Medical Travel Awards for Best Marketing Initiative – Winner
2016: IMTJ Medical Travel Awards for Best Marketing Initiative – Winner
2016: IMTJ Medical Travel Awards for International Hospital of The Year – Highly Commended
2016: Global Brands Magazine Awards 2016- Most Innovative Health Care Brand 2016, Malaysia
2016: Elite Member of Malaysia Healthcare Tourism Council
2016: CHT Pursuit of Excellence Award 2016 – Medical
2015: HR Vendors of The Years 2015 – Silver Award for Best Corporate Healthcare Provider
2015: Brand Excellence in Healthcare – Hospital
2015: The Brandlaureate Special Edition World Awards – Brand Excellence in Healthcare – Hospital
2015: IMTJ Medical Travel Award : Excellence in Customer Service
2014: IMTJ Medical Travel Award
2012: The Best of Malaysia Service to Care Champion 2012
2011: The Most Trusted Brand Award by Reader’s Digest
2011: Malaysian Service to Care Champion 2011
2010: Member of International Wellness & Healthcare Travel Association (IWHTA)
2009: Malaysian Branded Service Champion, Hospital Category
2007: Health Industry Recognition Award, by the Ministry of Health, Malaysia
2007: Asian Hospital Management Award (marketing, public relations, or promotional project category)
2007: Reader’s Digest as the Most Trusted Brand Award (hospital category)
2006: Asia Spa Wellness Awards for Technology Business Review (holistic patient care category) and Best Hospital
Hospital of The Year in Malaysia, Thank you for believing in us!
Gleneagles Hospital Kuala Lumpur made a commitment to improve the health and wellbeing of its patient and communities. To accomplish this, we are on a mission to continuously raise the bar in clinical, operational, and service excellence to always provide the highest standard of care.
The GlobalHealth Asia-Pacific Awards 2022 presented 4 awards to Gleneagles Hospital Kuala Lumpur, including the coveted Hospital of the Year in Malaysia award, recognising of our accomplishments and consistency in implementing various initiatives and patient-centric strategies towards improving health over the past years.
“These awards are a testament to the hard work and skills of our experienced doctors and staff, truly showcasing our dynamic leadership and our commitment to healthcare excellence,” says Gleneagles Hospital Kuala Lumpur’s Chief Executive Officer, Hoo Ling Lee.
“We will continuously strive to give our patients and their loved one’s peace of mind by providing the best care and treatment through comprehensive infrastructure, technology and services.”


Contact Information
Pantai Medical Centre Sdn Bhd (Registration No.: 198101006941 (73056-D)).
All Rights Reserved. Photos are for illustration purposes only
KKLIU 3489 / EXP 31.12.2025
EMERGENCY CONTACT
Gleneagles Hospital Kuala Lumpur
Ambulance / Emergency
+603 4141 3018
Select a hospital








.jpg?sfvrsn=13b534e1_1)







